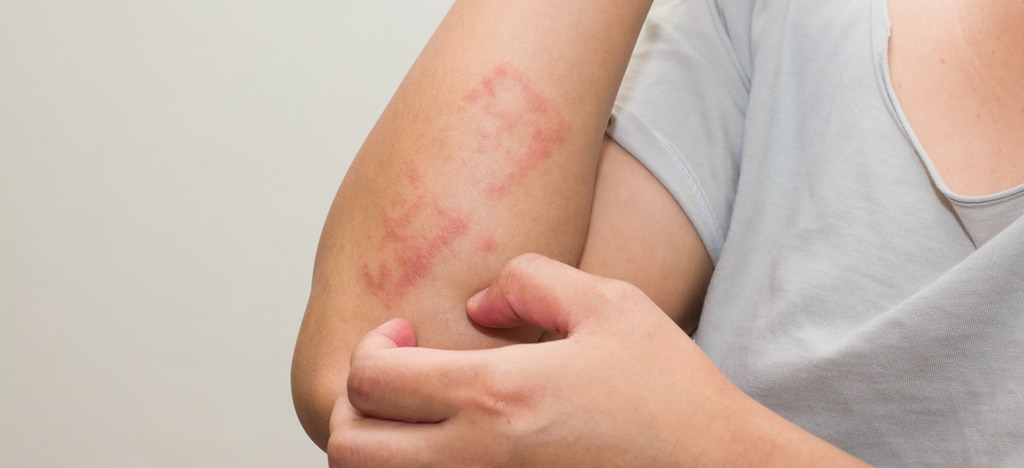
What is Psoriasis?
Psoriasis is a non-contagious inflammatory skin condition. It typically shows up as red and scaly plaques which are areas of thickened skin. It is a chronic skin disease that comes and goes, fluctuates in severity and itching is commonly associated with it. There is a genetic predisposition to psoriasis and may be associated with inflammatory arthritis. It is often triggered by infection, injury or psychological stress.
Who suffers from Psoriasis?
Psoriasis affects about 2-4% of the population and about one third of people with psoriasis have family members with psoriasis. The age of onset can be from childhood to elderly with peaks of onset at 15-25 years and 50-60 years.
What causes Psoriasis?
Psoriasis is caused by the rapid growth and turn over of the skin cells, resulting in red, thickened areas of the skin with scales. The cause is not fully understood, it appears to be related to the immune system and inflammatory process.
The normal life cycle of skin cells is about 1 month whereas in psoriasis, the life cycle is accelerated and shortened to about 1 week, resulting in redness, itch, buildup of extra skin cells which forms scales and thickening of the skin. This accelerated process is similar to the pattern of healing wounds. The immune & inflammatory cells are normally involved in dealing with wounds and infection. In psoriasis, these cells attack the healthy skin cells by mistake and trigger the inflammatory and healing process which causes the skin reaction seen in psoriasis. It is not entirely clear what causes these immune and inflammatory cells to malfunction.
Psoriasis can occur with no obvious cause and often can be induced or worsen by certain triggers. The triggers may include infection, injury, physical or psychological stress, smoking, excessive alcohol, certain medications, vitamin D deficiency.
What are the symptoms of Psoriasis?
There are different types of psoriasis, the most common is known as chronic plaque psoriasis, which appears as areas of red thickened skin with scales. Other symptoms & signs that may occur include itching, dry cracked skin, thickened pitted or ridged nails, pustules are seen in Pustular Psoriasis. 5-15% may have arthritis with swollen & stiff joints. Psoriasis patches can range from a few small areas of red scaling to large areas of skin eruption. The most common sites are scalp, elbows, knees but any part of the skin can be involved. Smooth patches are seen in Inverse Psoriasis which affects the skin in the armpits, groin, genital areas.
What is the treatment for Psoriasis?
Psoriasis is a chronic skin condition with flare ups and remissions. The aim is to prevent flare ups and worsening of the condition. Avoiding the triggers (such as smoking, excessive alcohol), managing stress, getting enough sun exposure to prevent Vitamin D deficiency would help. While there is no cure for psoriasis, the symptoms can be managed. Some people remain in remission for long periods of time.
Treatment is based on severity and types of psoriasis as well as the individual’s response to the medication used. Regular moisturizing helps to reduce itch & scales. Topical treatment (using moisturizer and topical agents) is usually sufficient to control mild psoriasis. More severe psoriasis may require phototherapy.
Oral medication may be added if severe psoriasis is not responding to phototherapy. Oral medication has side effects and would regular monitoring with blood tests. Newer available therapy includes use of biologics which are reserved for severe psoriasis that are resistant to treatment.
Psoriasis can affect quality of life & self esteem which can result in social withdrawal and depression. Managing the physical and the psychosocial aspects of psoriasis have made it possible for people to live with effects of psoriasis.
 Dr Sin Ru Phua is based at IMC Camden and has GDFPDerm in Dermatology.
Dr Sin Ru Phua is based at IMC Camden and has GDFPDerm in Dermatology.
For an appointment please call 6733 4440 or click here: https://www.imc-healthcare.com/appointments/